Can a Second Conversation Save Millions?
An episode of care usually starts when a patient begins receiving that care. But in the world of benefits, the most impactful work happens before that episode ever begins. When surgery is treated like a foregone conclusion for muskuloskeletal disorders, it's worth asking the question that one client did: Is rising surgical spend truly unavoidable?
Read on to:
- See how episode-of-care cohorts helped quantify cost differences across common surgery-treated conditions
- Explore how member behavior—specifically low second-opinion utilization—impacted PMPM and total spend
- Learn how these insights helped an employer build the business case for a second-opinion benefit program

Overview
Many self-insured employers are looking for ways to reduce the cost of an episode of care, whether it’s by bundling payments, using centers of excellence, or steering members toward second opinion benefits. Second opinion benefit programs help members seek another doctor’s opinion before surgery or other major procedures to ensure they’re getting the best advice. But, this can be both pricey, too. So how can an employer determine if standing up a second opinion service for their members is worthwhile?
A large self-insured employer with a handful of high cost conditions came to us with exactly this question.
The Discovery
To answer their question effectively, we first grouped claims into clinical cohorts across five common surgery-treated conditions: cervical disc disorders, degenerative joint disease (hip and knee), low back pain, and obesity. Using episode-of-care methodology, our client could finally compare spend, utilization, and member behavior across diagnoses. Here are some of the highlights of our key findings:
.png)

In summary:
- Members with these conditions had significantly higher PMPM costs. For example, cervical disc disorder members had ~3x higher PMPM than those without the diagnosis.
- Surgery was common, but second opinions were not. Out of 116 members treated for knee degenerative joint disease, 50 had surgery, but only 1 sought a second opinion beforehand.
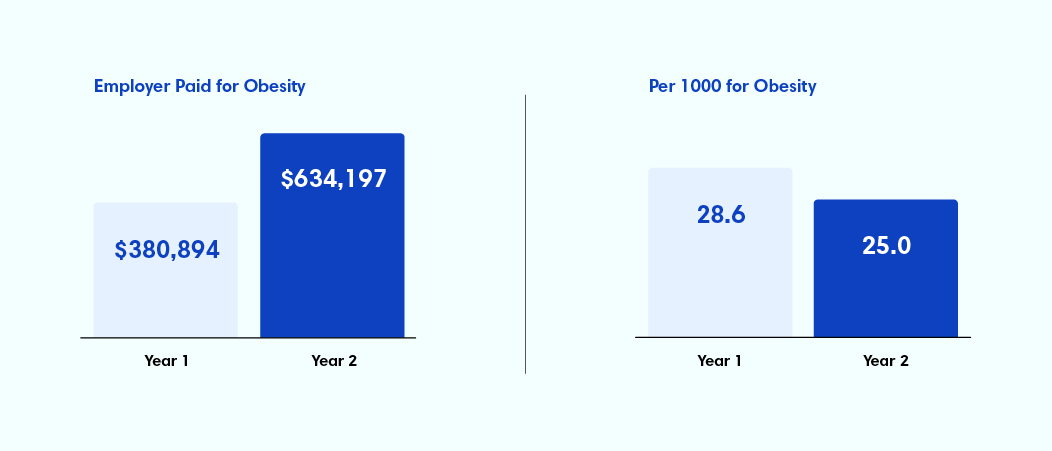
- Costs were shifting in unexpected ways. While obesity prevalence slightly declined, employer-paid spend for obesity nearly doubled from $380K to $634K year over year.
The Domino Effect
Spotlighting some of these conditions indicated an early opportunity to reverse a trend toward higher costs, like in the case of obesity. It also revealed nearly no utilization of a second opinion, like in the case of joint disease.
Low second-opinion utilization meant members were proceeding directly to surgery without confirming necessity, appropriateness, or lower-cost alternatives, and there was certainly an opportunity to bridge the gap. The downstream effects included:
- Higher surgical rates and associated downstream rehab costs
- Missed opportunities for conservative treatment or step therapy
- Rising spend even in conditions where prevalence was stable
- Member experience risks (e.g., facing surgery without confidence in the recommendation)
- Loss of productivity due to surgery
The Action Plan
Artemis helped the employer build a data-driven justification for implementing a formal second-opinion benefit, using insights from the episode-of-care review. The employer is moving forward with implementing a second-opinion benefit that will:
- Educate members on treatment options before they choose surgery
- Provide a point of contact for next step care navigation for musculoskeletal and metabolic conditions
- Provide a guide for finding in-network doctors, therapies, and surgeons
The Outcome
With better education around alternative care options and assistance with care navigation, the employer hopes to improve care quality and confidence in treatment pathways and reduce spend across high-cost musculoskeletal and metabolic conditions. As these interventions roll out, Artemis will help monitor the program’s success, as indicated by changed member behavior, better care alignment, and a decrease in avoidable surgical spend.
The Takeaway
Understanding the full cost of a condition (and where the cost drivers are) is critical to implementing targeted solutions to address avoidable high-cost claims. In this case, episode-of-care analytics also revealed member behaviors and year-over-year shifts that would have otherwise gone unnoticed.
