How Paychex Uncovered $1.5M in Avoidable ER Spend—And Turned Data Into Swift Action
High-level ER metrics rarely explain why members go or where costs could have been avoided. Using meaningful insights in the Artemis Platform, including avoidable ER metrics, Paychex identified a clear opportunity. They partnered with Artemis to look beyond surface-level utilization and understand how targeted actions could steer members toward the right care, at the right time, and at the right cost.
Read on to:
- See how Paychex quantified avoidable ER visits using our clinically validated data models
- Understand which locations and conditions were specifically driving unnecessary ER spend
- Learn how targeted education and telemedicine strategies can change member behavior
.png)
Overview
Paychex, a leading provider of integrated human capital management solutions, supports approximately 670,000 payroll clients and pays one of out every 12 private-sector employees in the U.S. Paychex's benefits team noticed they had an opportunity to save costs on emergency room claims, an opportunity that has existed for a number of years. They partnered with Artemis Health to look more closely at their benefits data, and they saw that avoidable emergency room claims accounted for a staggering $1.5 million in their spending in the first half of 2019.
The Discovery
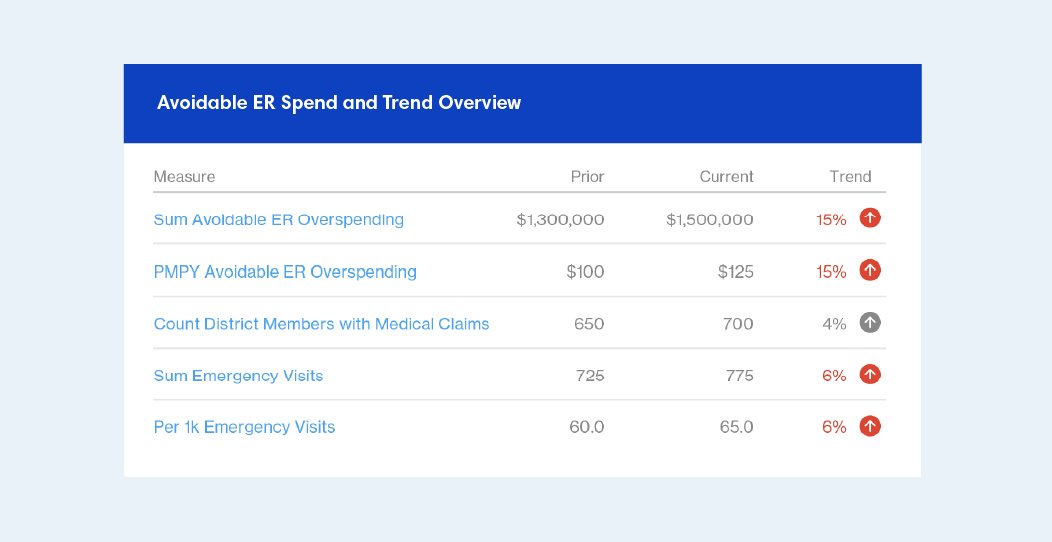
Not only was ER spend very high, but it was also trending up. Members were visiting the ER more often, in large numbers for each analysis period, and the cost was rising for both Paychex and members.
While some conditions really do require emergency care, Artemis uses a clinically validated1 data model to flag certain types of visits as “avoidable.” The Artemis Platform automatically calculates the total cost that could have been saved if all claims had been handled at the correct point of care.
To move from insight to action, Paychex went deeper into the data to understand where and why avoidable ER visits were occurring.
.png)
What Artemis helped uncover:
- Avoidable ER utilization varied significantly by office location
- Offices with the highest enrollment were not always the highest ER cost drivers
- Certain locations emerged as clear hotspots for inappropriate ER use
The team also analyzed which conditions were driving avoidable visits. Common diagnoses included:
- Urinary tract infections
- Headaches
- Cough
- Low back pain
- Nausea
The Action Plan
Armed with this clarity, Paychex began designing targeted interventions, including:
- More aggressively promoting telemedicine, ensuring employees understood their options for immediate care
- Sending targeted member education to office locations with higher avoidable ER costs—tailored by demographics and visit drivers
- Conducting on-site benefits education sessions to reinforce when and where to seek care (with timing adjusted due to COVID-19)
The Outcome
While some initiatives were delayed due to the COVID-19 pandemic, the analysis itself immediately changed how Paychex approached ER utilization. Telemedicine awareness increased, and the benefits team gained a data-backed roadmap for addressing inappropriate care patterns once in-person education could resume.
More importantly, Paychex shifted from reacting to ER costs to proactively managing them—using data to guide smarter member behavior and more intentional benefits strategies.
The Takeaway
These cost-saving strategies aren’t just impactful for the business; Paychex is also empowering employees to make smart healthcare decisions, save the plan money, and save money on out of pocket costs as well. By tackling high ER utilization with targeted member education efforts, Paychex is incentivizing good healthcare decisions for employees and their families. It’s all part of their effort to get employees to get the right care, at the right time, at the right place, for the right cost.
---
1Based on a NYU Wagner study around emergency room utilization.
