Is 'GLP-1 Seeking Behavior' Blowing Up Your Budget?
When diabetes diagnoses start climbing, it's natural to assume your population is getting sicker. But as employers began tightening coverage for GLP-1s, Artemis noticed something worth a closer look. In this case study, you’ll see how Artemis uncovered GLP-1-seeking behavior hidden in the data and helped an employer put the right guardrails in place to manage costs without limiting appropriate care.
Read on to:
- See how Artemis connected first-time diabetes diagnoses with first-time GLP-1 prescriptions
- Explore how member behavior can shift in response to benefit design and coverage rules
- Learn how data-driven insights helped align policy, prescribing, and spend

Overview
GLP-1s like Ozempic, Wegovy, and Mounjaro have become household names. There haven’t been many other prescription drugs in recent history that have made its way into mainstream culture quite the way GLP-1s have, popularized by celebrities and doctors (and, celebrity doctors) alike. For employers, that sort of notoriety has been reflected in their bottom line. And it leaves us asking the question—has the need driven the hype, or has the hype driven the “need”?
We helped one of our clients, a globally recognized insurance company covering more than 50,000 lives, dig a little deeper when we noticed a concerning trend.
The Discovery
As Artemis analysts reviewed year-over-year trends, one data point stood out: a 30% jump in Type 2 Diabetes prevalence.
That spike came at the same time many employers were tightening access to GLP-1 medications (limiting their usage as treatment only for diabetes and requiring prior authorizations or step-therapy for diabetes use). Also of note:
- In this client’s population, there were no prior risk factors or historical indicators of diabetes in these members’ claims, in most instances.
- Members receiving GLP-1s for the first time were diagnosed with diabetes for the first time as well.
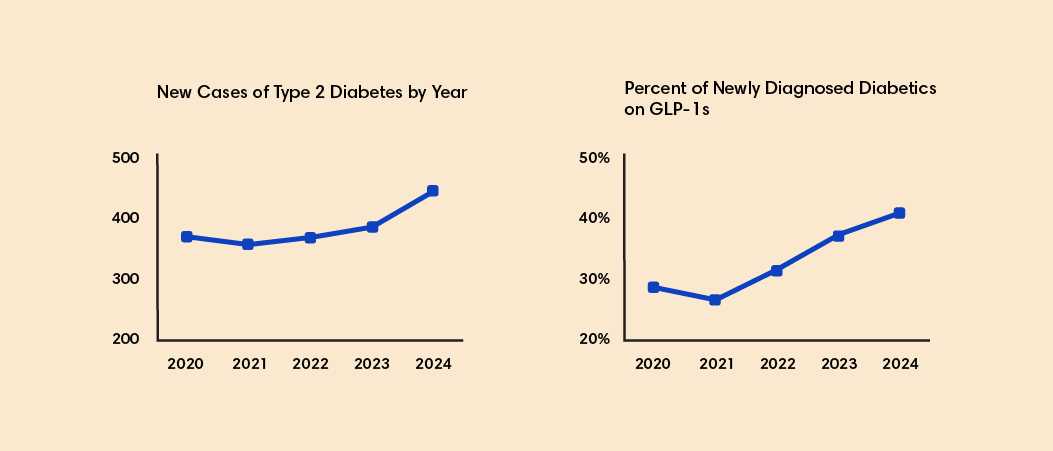
The trend raised a red flag. Were some new diabetes diagnoses being made as a means of accessing GLP-1 therapy through covered channels, rather than reflecting true disease onset?
The Domino Effect
GLP-1s are among the most expensive drug classes on the market. Over-utilization means millions in unnecessary spend, not to mention misaligned prescribing undermines plan design and drives up premiums for all members. Left unchecked, this prescribing trend would have caused costs to balloon without clinically indicated benefit.
The Action Plan
We partnered with the client to validate the pattern and take steps to protect both clinical integrity and plan design. The response focused on three core areas:
- Conducting a targeted claims audit: Artemis analyzed batches of medical and pharmacy claims to identify clusters for first-time GLP-1 prescriptions paired with new diabetes diagnoses, assess whether members had historical markers or risk factors for diabetes, and surface providers whose diagnostic and prescribing patterns deviated significantly from peers. This helped us distinguish appropriate clinical care from potential GLP-1 seeking behavior.
- Collaborating with the PBM to review approval pathways: We worked directly with the client’s PBM to examine prior authorization criteria, step-therapy enforcement, and possible loopholes allowing GLP-1 access without evidence of disease prevention.
- Strengthening controls to support appropriate use: Based on the findings, the client implemented refinements, such as updated documentation requirements for diabetes diagnoses tied to GLP-1 initiation, tighter verification steps to confirm clinical indications before approval, and clearer communication to providers on evidence-based prescribing expectations.
The goal wasn’t to restrict access, but to make sure the right members received the right therapies for the right reasons.
The Outcome
As a result of this analysis and intervention, the client achieved:
- Better policy alignment between PBM and employer goals
- Fewer unnecessary GLP-1 prescriptions
- Reduced waste and overspending, preserving resources for members who truly need advanced therapies
“This is a perfect example of using data not just to monitor spend, but to correct it in real time.”
— Client Stakeholder
The Takeaway
Employer experiences with GLP-1s are just the beginning. As new medical advancements and gene therapies enter the market, unexpected utilization patterns, and the incentives behind them, will become more common, not less.
Data gives employers the early warning system they need to anticipate member behavior, evaluate incentives, and course-correct before cost trends take off.
As employers revisit their plan designs, they should be proactively establishing clear frameworks for:
- whether to provide coverage for high-cost therapies,
- what guardrails must be in place when coverage is offered, and
- which administrative systems can enforce those standards consistently and transparently.
