Selecting a Solution to Manage Type II Diabetes
One employer suspected that Type II diabetes was having a larger impact on their health plan than surface-level metrics suggested—and that their benefits strategy could do more to support members managing the condition. In this case study, see how analytics helped validate assumptions, inform intervention, and guide solution selection.
Read on to:
- See how diabetes prevalence and cost appeared in the data
- Understand how high-cost claimants influence more than just the budget
- Learn how success of a solution was defined and measured over time
.png)
Overview
A large U.S. employer in the logistics industry, with more than 20,000 employees nationwide, knew that Type II diabetes was a major cost driver in their health plan. But rising spend was only part of the concern. Leadership wanted to understand how diabetes was affecting employee health, engagement, and long-term outcomes—and whether their benefits strategy was truly supporting the members who needed it most.
They partnered with Artemis Health to uncover what was happening beneath the surface and identify opportunities to intervene more effectively.
The Discovery
Artemis analyzed claims and enrollment data for members with a medical diagnosis of Type II diabetes or prescriptions related to diabetes management. The analysis also layered in demographic factors like age, gender, and geography to better understand who was most likely to engage with available benefits.
Our findings showed that:
- Members with Type II diabetes were incurring 2.5x higher costs than non-diabetic members
- Diabetes rarely appeared in isolation; comorbid conditions were common and compounding costs
- A significant portion of overall plan spend was being driven by a relatively small population
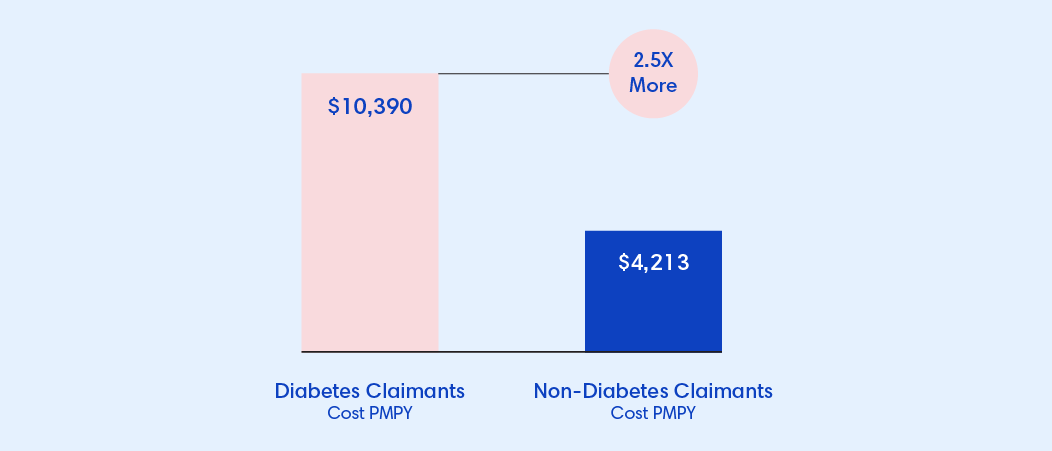
The Domino Effect
Higher utilization, unmanaged comorbidities, missed primary care visits, and inconsistent medication adherence all contribute to avoidable spend and poorer member experience. For this employer, diabetes wasn’t just a line item on a cost report. It was quietly shaping productivity, employee wellbeing, and future financial risk.
The Action Plan
The customer, along with their consultant partners, used this data to justify a more targeted diabetes care management solution.
Together, they:
1: Selected a diabetes point solution that provided:
- Diabetes testing and monitoring
- Personalized coaching and ongoing support
2: Defined Measurable Goals
Before rollout, Artemis helped establish clear benchmarks to track progress over time, including:
- Enrollment rates
- Medication adherence
- Primary care engagement
- Member satisfaction
3: Designed a Multi-Channel Engagement Strategy
The program launch was supported through:
- Targeted emails and printed materials
- Quarterly benefits meetings
- Reinforcement during Open Enrollment
.png)
The Outcome
Over the past two years, the customer has kept an eye on the point solution using Artemis Health’s data analytics. Here are the results:
- 32% of eligible members enrolled in the program
- 89% medication compliance among participants
- 10% improvement in primary care visits
- 91% member satisfaction with the program
While enrollment and PCP visits fell slightly short of their goals, medication adherence and satisfaction exceeded expectations, signaling that members with Type II Diabetes were engaging with their health and this new benefit program. The customer is pleased with their results and will continue to use Artemis to monitor their success. Their next ambitious goal: a 15% reduction in costs for members with diabetes.
